A vast number of studies examined the effects of environmental noise on sleep, and there are different methods to measure sleep.
1. The most comprehensive methodology to physiologically assess sleep is so-called polysomnography (PSG), which encompasses various measurements, including electrophysiological assessment of brain activity (electroencephalogram, EEG), eye movement (electrooculogram, EOG), heart activity (electrocardiogram, ECG), as well as muscle activity (electromyogram, EMG).
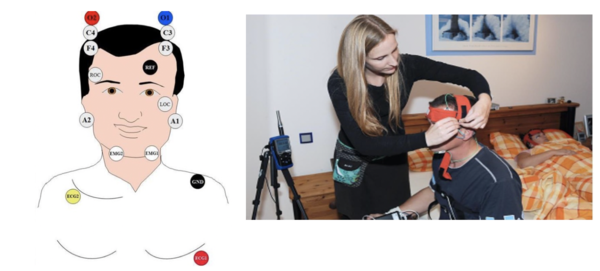
Figure 1: Schematic representation of the electrode positioning for the measurement of polysomnography (source: DLR)
Figure 2: Preparing subjects for polysomnographic recordings (source: DLR)
2. A less invasive method for participants is actigraphy, which measures a person's body movements via a single device worn on the wrist. In recent studies, authors attempted to use the combination of actigraphy and ECG measurements in order to detect awakenings in a less costly way than employing PSG.
3. Next to physiological measurements, there is also the option to ask participants about their experience of sleep disturbances or sleep quality, i.e. a psychological assessment of sleep. The items used for this type of assessment can refer to the last night's sleep or a participant's sleep experience over a more extended period. Estimates using questionnaires are relatively cheap and easy to implement. Numerous published examples have been used for calculating 'mean' exposure-response curves of 'at least a little sleep disturbed', 'sleep disturbed' and 'highly sleep disturbed' people over an energy equivalent noise level LNight. In March 2020, the new Directive EU 2020/367 was published providing the basis for the calculation of the number of highly sleep-disturbed residents depending on the nocturnal aircraft noise level as well as for the estimation of the total number of people affected by high aircraft noise-induced sleep disturbance. However, research has shown that psychological assessments do not necessarily reflect physiologically measured sleep disturbances and interruptions.
A fundamental problem with exposure response curves based on equivalent levels, is that those 'mean' levels, if not unrealistically low, are not suitable for communication to communities or for protection purposes for noise effects on sleep as many different noise situations can lead to the same Leq and have different effects on sleep. The World Health Organisation recommends in its "Environmental Noise Guidelines for the European Region" (2018) an LNight threshold of 40 dB(A) for aircraft noise due to the number of 'Highly Sleep Disturbed people' (HSD), assessed by questionnaires (WHO, 2018). In reality, a Boeing 747 on take-off with a distance of 10 km from the runway, 600 m height, one movement per 8 hours already would lead to an LNight of 51 dB(A), or for an Airbus 320, 10 km distance from the runway on take-off, 770 m height, eight movements per 8 hours would lead to an LNight of 50 dB(A).